MSC THERAPY FOR METABOLIC CONDITIONS
Neurological & developmental conditions where MSC therapy has been studied or explored as supportive care at KSAA STEMCARE
Type 1 diabetes
Diabetic neuropathy
Diabetic foot ulcer
Impaired glucose metabolism
Type 2 diabetes
Diabetic cardiomyopathy
Chronic inflammation
Metabolic syndrome
How does MSC therapy aid in Metabolic conditions
Stem cell therapy addresses metabolic conditions (most notably diabetes) by targeting the root causes of the disease—cellular damage, inflammation, and insulin dysfunction—rather than just managing blood sugar levels. Here is a breakdown of the biological mechanisms by which stem cells help in metabolic conditions.
1. Regeneration of Pancreatic Beta Cells
a. Differentiation (Creating New Cells)
Some stem cells, especially Induced Pluripotent Stem Cells (iPSCs), have the ability to develop into many different cell types. This includes the potential to become new insulin-producing beta cells, which are the cells in the pancreas responsible for making insulin.
b. Cell Rescue (Supporting Existing Cells)
In adults, the type of stem cells most commonly used are Mesenchymal Stem Cells (MSCs). Instead of turning into new beta cells, MSCs work in a different way — they may help repair and support existing beta cells that are weak, inflamed, or not functioning properly.
MSCs do this by releasing natural healing signals that may reduce inflammation, support tissue recovery, and encourage damaged beta cells to become more active again.
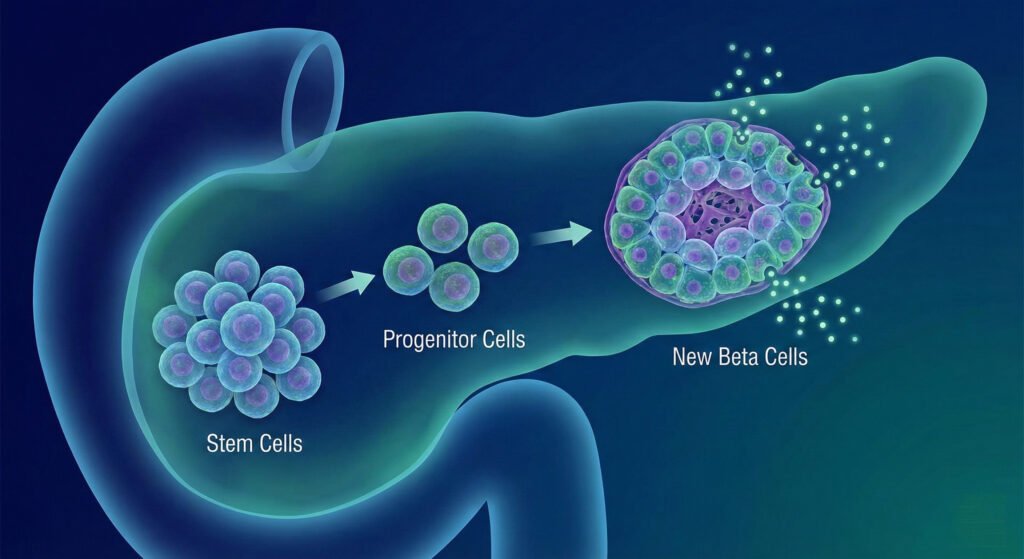
In both Type 1 and Type 2 diabetes, the beta cells in the pancreas (which produce insulin) are either destroyed or damaged.
2. Immunomodulation (Stopping the Attack)
a. Type 1 Diabetes (Autoimmune):
The immune system attacks the pancreas. Stem cells release anti-inflammatory cytokines that can “reset” the immune system, halting the autoimmune attack and preserving remaining beta-cell function.
b. Type 2 Diabetes & Metabolic Syndrome:
These conditions are fueled by systemic, low-grade inflammation (often from adipose/fat tissue). Stem cells reduce this systemic inflammation, which is a primary cause of insulin resistance.
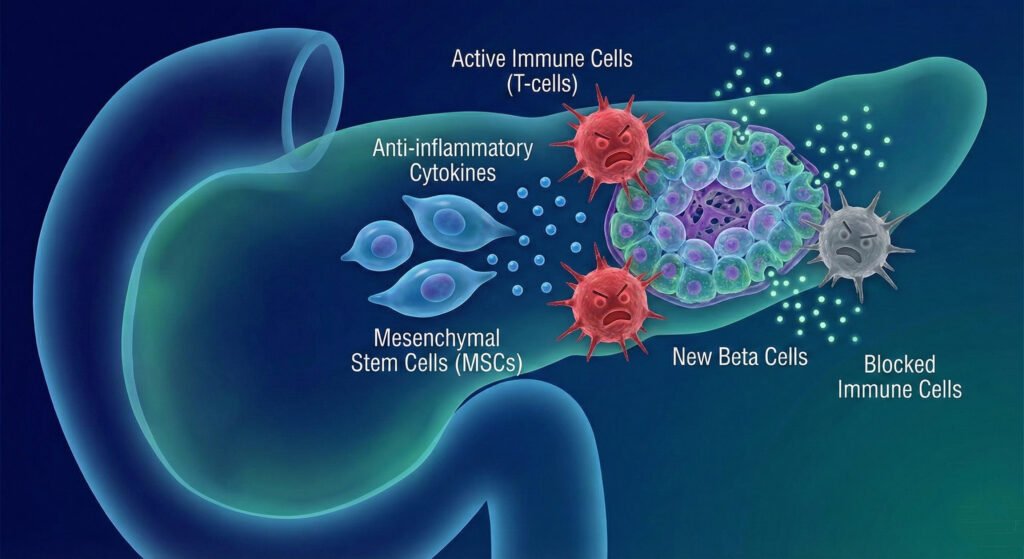
Chronic inflammation is a key driver of metabolic failure.
3. Reversing Insulin Resistance
a. Sensitivity Boost:
Stem cells improve the sensitivity of peripheral tissues (muscle, liver, and fat) to insulin. This allows cells to absorb glucose from the bloodstream more efficiently, lowering blood sugar levels naturally.
b. Signaling Repair:
They repair the signaling pathways that tell cells when to store or burn energy, helping correct metabolic imbalance.
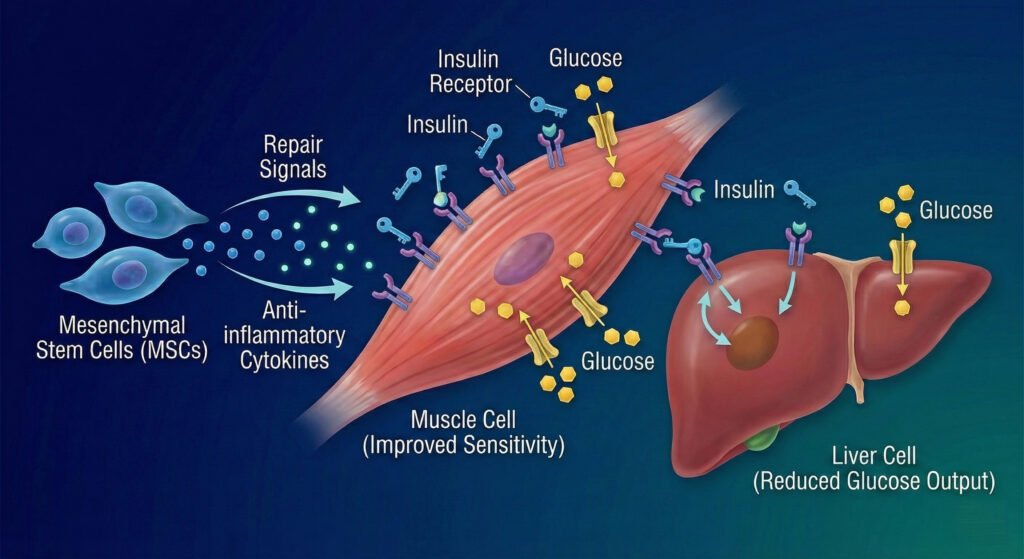
In both Type 1 and Type 2 diabetes, the beta cells in the pancreas (which produce insulin) are either destroyed or damaged.
4.Paracrine Signaling (The Halo Effect)
a. Promote angiogenesis:
(Growth of new blood vessels) to improve circulation to damaged organs.
b. Prevent cell death:
(Apoptosis) in the pancreas and kidneys.
c. Reduce fibrosis (scarring):
In organs affected by high blood sugar, such as the liver and kidneys.
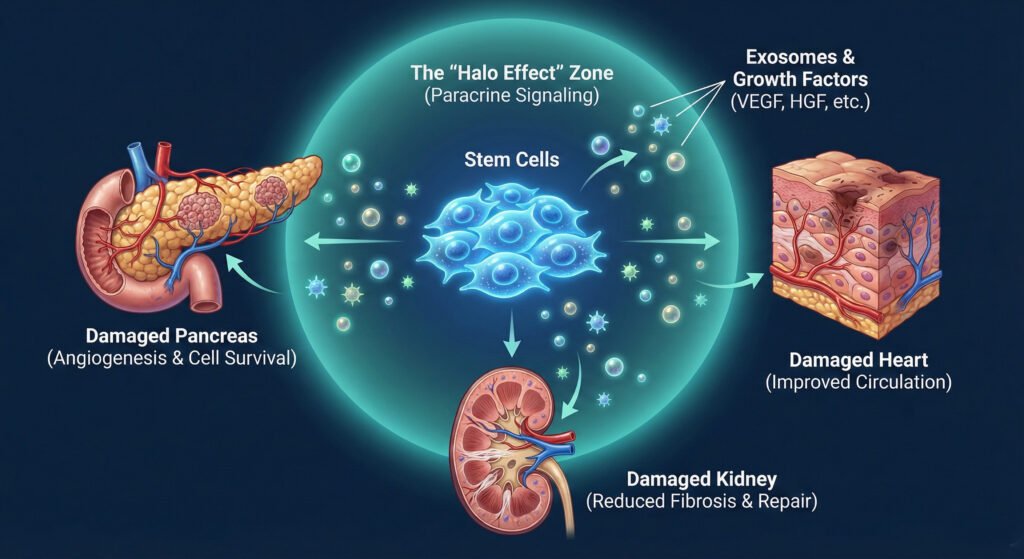
In both Type 1 and Type 2 diabetes, the beta cells in the pancreas (which produce insulin) are either destroyed or damaged.
1. Regeneration of Pancreatic Beta Cells
a. Differentiation (Creating New Cells):
Some stem cells, especially Induced Pluripotent Stem Cells (iPSCs), have the ability to develop into many different cell types. This includes the potential to become new insulin-producing beta cells, which are the cells in the pancreas responsible for making insulin.
b. Cell Rescue (Supporting Existing Cells):
In adults, the type of stem cells most commonly used are Mesenchymal Stem Cells (MSCs). Instead of turning into new beta cells, MSCs work in a different way — they may help repair and support existing beta cells that are weak, inflamed, or not functioning properly.
MSCs do this by releasing natural healing signals that may reduce inflammation, support tissue recovery, and encourage damaged beta cells to become more active again.

In both Type 1 and Type 2 diabetes, the beta cells in the pancreas (which produce insulin) are either destroyed or damaged.
2. Immunomodulation (Stopping the Attack)
a. Type 1 Diabetes (Autoimmune):
The immune system attacks the pancreas. Stem cells release anti-inflammatory cytokines that can “reset” the immune system, halting the autoimmune attack and preserving remaining beta-cell function.
b. Type 2 Diabetes & Metabolic Syndrome:
These conditions are fueled by systemic, low-grade inflammation (often from adipose/fat tissue). Stem cells reduce this systemic inflammation, which is a primary cause of insulin resistance.

Chronic inflammation is a key driver of metabolic failure.
3. Reversing Insulin Resistance
a. Sensitivity Boost:
Stem cells improve the sensitivity of peripheral tissues (muscle, liver, and fat) to insulin. This allows cells to absorb glucose from the bloodstream more efficiently, lowering blood sugar levels naturally.
b. Signaling Repair:
They repair the signaling pathways that tell cells when to store or burn energy, helping correct metabolic imbalance.

In both Type 1 and Type 2 diabetes, the beta cells in the pancreas (which produce insulin) are either destroyed or damaged.
4.Paracrine Signaling (The Halo Effect)
a. Promote angiogenesis:
(Growth of new blood vessels) to improve circulation to damaged organs.
b. Prevent cell death:
(Apoptosis) in the pancreas and kidneys.
c. Reduce fibrosis (scarring):
In organs affected by high blood sugar, such as the liver and kidneys.

In both Type 1 and Type 2 diabetes, the beta cells in the pancreas (which produce insulin) are either destroyed or damaged.
Get a Free Consultation for MSC Treatment Now!
Consult with our experienced professionals today and take the first step toward a healthier life.
Get a Free Consultation for MSC Treatment
Consult with our experienced professionals today and take the first step toward a healthier life.

